Healthcare organizations across the world are facing increasing financial and operational pressure due to rising patient volumes, complex payer regulations, and growing administrative workloads. Traditional billing systems that rely heavily on manual data entry and fragmented workflows are no longer capable of supporting modern hospital operations efficiently. From coding inaccuracies and delayed reimbursements to insurance claim denials and disconnected billing systems, hospitals continue to lose significant revenue because of inefficient financial processes.
This growing complexity has accelerated the adoption of AI medical billing solutions and intelligent healthcare automation platforms across hospitals, clinics, and multi-specialty healthcare networks. Modern AI agents are transforming the way healthcare providers manage insurance claims automation and healthcare revenue cycle management by reducing repetitive administrative tasks, improving billing accuracy, and streamlining reimbursement workflows.
Unlike conventional hospital billing software, AI-powered systems can analyze large volumes of financial and patient data in real time, helping hospitals detect coding errors, verify insurance eligibility, automate claim submissions, and predict claim denial risks before they impact revenue. As healthcare organizations continue investing in digital transformation strategies, AI-driven financial automation is becoming a critical component of sustainable hospital operations.
The growing impact of AI Agents Are Transforming the Healthcare Industry is now extending beyond clinical care into revenue cycle optimization, helping healthcare providers improve operational efficiency while strengthening long-term financial performance.
Understanding Medical Billing and Revenue Cycle Challenges in Modern Hospitals
Managing healthcare revenue cycle management has become increasingly difficult for hospitals operating in today’s highly regulated and data-intensive healthcare environment. Medical billing departments are expected to process large volumes of insurance claims accurately while simultaneously complying with constantly evolving payer rules, coding standards, and healthcare regulations. Even minor documentation or coding errors can result in claim denials, delayed reimbursements, and substantial revenue losses for healthcare organizations.
One of the biggest challenges hospitals face is the complexity of insurance claims processing workflows. Every insurance provider follows different authorization procedures, reimbursement structures, and documentation requirements. Billing teams often spend countless hours manually verifying patient eligibility, validating coverage information, correcting claim discrepancies, and tracking unpaid claims. These repetitive administrative tasks significantly slow down reimbursement cycles and increase operational inefficiencies.
Prior authorization delays have also become a major burden for healthcare providers. Manual approval processes can postpone treatments, delay claim submissions, and negatively impact both patient satisfaction and hospital cash flow. In large healthcare systems, disconnected hospital billing software and siloed financial systems further complicate revenue management by limiting visibility across departments.
Human coding errors remain another major contributor to claim rejections and revenue leakage. Incorrect CPT or ICD coding can trigger compliance risks, audits, and payment denials that require additional administrative effort to resolve. As patient volumes continue to rise, hospital finance teams are increasingly struggling with staff burnout caused by excessive workloads and repetitive billing responsibilities.
Healthcare providers are now under immense pressure to modernize their insurance claims processing systems while maintaining compliance, operational accuracy, and financial stability. This growing need for intelligent automation is driving hospitals toward AI-powered financial technologies that can improve revenue cycle efficiency while reducing administrative complexity.
What Are AI Agents in Medical Billing and Claims Management?
AI agents in healthcare are intelligent software systems designed to automate complex operational tasks, make data-driven decisions, and continuously optimize workflows with minimal human intervention. In medical billing and claims management, these AI-powered systems are transforming how hospitals handle financial operations by improving speed, accuracy, and scalability across the entire revenue cycle.
Traditional automation tools typically follow fixed rules and repetitive workflows. While they can automate basic tasks such as form generation or data entry, they often fail when workflows become more dynamic or require contextual decision-making. AI agents, however, use machine learning, natural language processing (NLP), predictive analytics, and real-time data analysis to manage complex billing and insurance processes intelligently.
Modern AI claims processing systems can independently verify insurance eligibility, analyze patient records, detect coding anomalies, automate claims submission, monitor reimbursement status, and identify high-risk claims before submission. These intelligent systems continuously learn from historical billing data, payer behavior, and reimbursement trends, allowing hospitals to optimize financial workflows more effectively over time.
One of the biggest advantages of intelligent healthcare automation is its ability to execute autonomous workflows in real time. AI agents can instantly flag incomplete documentation, recommend billing corrections, validate insurance information, and route claims to the correct payer systems without requiring constant human supervision. This significantly reduces administrative burdens on billing teams while improving operational efficiency.
As healthcare organizations continue adopting advanced digital infrastructure, the role of intelligent AI systems in financial management is expanding rapidly. Hospitals are increasingly investing in Compliant AI Agent in Healthcare solutions and advanced agent ai development services to build scalable billing ecosystems capable of supporting modern healthcare operations while ensuring security, compliance, and long-term revenue optimization.
How AI Agents Automate Insurance Claims Processing in Hospitals
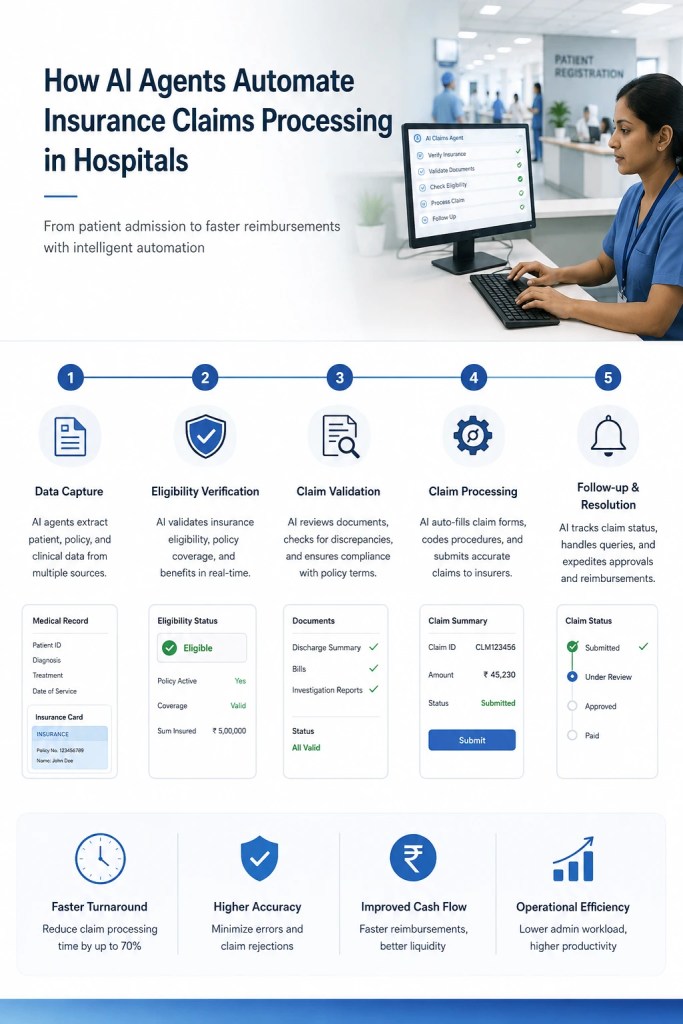
Insurance claims processing is one of the most complex and resource-intensive functions within hospital financial operations. Traditional workflows often involve multiple departments, manual documentation checks, repetitive data entry, and constant communication with insurance providers. These fragmented processes not only slow down reimbursements but also increase the likelihood of coding errors, claim denials, and revenue leakage. AI-powered medical billing systems are transforming this entire workflow by introducing intelligent automation at every stage of the claims lifecycle.
The automation process typically begins during patient registration. AI agents can automatically capture patient demographics, validate insurance details, and verify eligibility in real time before treatment even begins. This reduces front-desk administrative workload while minimizing errors caused by incomplete or outdated patient information. Automated insurance validation also helps hospitals identify coverage limitations and authorization requirements early in the patient journey.
Medical coding is another critical area where AI claims processing systems deliver significant value. AI-powered tools can analyze clinical documentation and recommend accurate CPT and ICD codes using natural language processing and machine learning algorithms. These systems help hospitals reduce coding inconsistencies, improve documentation accuracy, and maintain compliance with payer-specific billing regulations. Real-time error detection capabilities further reduce the risk of rejected claims caused by incorrect coding submissions.
Once coding is completed, AI agents automate the claims submission process by validating billing information against payer requirements before transmitting claims electronically. Intelligent validation checks ensure that missing documentation, duplicate claims, or formatting errors are identified before submission, improving first-pass claim acceptance rates significantly.
AI agents also play a major role in claims tracking and reimbursement monitoring. Instead of relying on manual follow-ups, hospitals can use intelligent systems to monitor claim status in real time, identify payment delays, and predict reimbursement risks using historical payer behavior patterns. Predictive delay detection allows billing teams to proactively address issues before they impact cash flow.
Denial management is one of the most valuable applications of insurance claims automation. AI systems can identify recurring denial patterns, analyze rejection reasons, and recommend corrective actions automatically. Some advanced platforms can even generate appeal recommendations and supporting documentation to accelerate dispute resolution.
By reducing manual intervention across the entire claims workflow, hospitals using AI-powered medical billing systems can improve operational efficiency, accelerate reimbursements, and achieve stronger claim denial reduction outcomes while optimizing overall financial performance.
Key Benefits of AI-Powered Medical Billing for Healthcare Providers
AI-powered medical billing is rapidly becoming a strategic priority for hospitals seeking to improve operational efficiency, financial stability, and long-term scalability. As healthcare systems continue facing increasing administrative complexity and reimbursement pressure, intelligent financial automation offers hospitals a more sustainable approach to managing modern revenue cycle operations.
One of the most immediate advantages of medical billing automation is faster reimbursement processing. AI agents can automate eligibility verification, claims validation, coding analysis, and payer submissions in real time, significantly reducing delays caused by manual workflows. Faster claim approvals directly improve hospital cash flow and reduce the financial burden associated with prolonged reimbursement cycles.
Reduced billing errors are another major benefit of intelligent healthcare workflow automation. Human errors in coding, documentation, and claims submission are among the leading causes of insurance claim denials. AI systems continuously analyze billing data for inconsistencies, missing information, and compliance risks before claims are submitted, helping hospitals improve billing accuracy and reduce costly rework.
Healthcare providers are also benefiting from lower administrative overhead. By automating repetitive financial tasks such as claims tracking, payment follow-ups, and denial management, hospitals can reduce the workload placed on billing staff and allocate resources more effectively. This not only improves productivity but also helps address staff burnout within revenue cycle departments.
Patient billing transparency is improving as well through AI-driven communication systems. Intelligent billing platforms can generate clearer payment summaries, automate billing notifications, and provide patients with faster responses regarding insurance coverage and outstanding balances. This creates a better financial experience for patients while reducing confusion and payment delays.
Another important advantage is enhanced compliance management. AI-powered systems continuously monitor payer regulations, coding updates, and healthcare compliance requirements, helping hospitals reduce audit risks and maintain operational consistency across departments.
Healthcare executives are increasingly prioritizing AI-driven hospital revenue optimization strategies because these technologies support long-term scalability. Multi-location hospitals and healthcare networks can manage large volumes of claims more efficiently while maintaining consistent financial operations across facilities. As healthcare organizations continue modernizing their digital infrastructure, intelligent automation is becoming a foundational component of sustainable revenue cycle management.
How AI Agents Reduce Insurance Claim Denials and Revenue Leakage
Insurance claim denials remain one of the biggest financial challenges for hospitals and healthcare providers. Even small billing inaccuracies can disrupt reimbursement cycles, increase administrative costs, and create significant revenue leakage over time. Traditional billing systems often struggle to identify errors before claims are submitted, forcing healthcare organizations to spend valuable time and resources correcting rejected claims manually.
Common causes of claim denials include incomplete patient documentation, incorrect CPT or ICD coding, eligibility mismatches, duplicate submissions, and missing prior authorizations. In high-volume healthcare environments, these issues can quickly accumulate and negatively impact hospital financial performance. Manual claims review processes are often unable to keep pace with increasing patient volumes and changing payer requirements, making denial prevention extremely difficult.
AI agents are transforming claim denial reduction by using predictive healthcare analytics and intelligent automation to identify potential risks before claims reach insurance providers. These systems analyze historical reimbursement data, payer behavior patterns, coding trends, and real-time billing information to detect anomalies that may result in denials. Instead of reacting to rejected claims after submission, hospitals can proactively resolve issues during the billing process itself.
Pattern recognition technology plays a major role in this process. AI systems can identify recurring denial trends linked to specific procedures, providers, insurance carriers, or documentation gaps. This allows hospitals to optimize workflows and improve billing accuracy continuously over time. Predictive risk scoring capabilities further help billing teams prioritize high-risk claims that require additional review before submission.
AI insurance verification systems also strengthen reimbursement accuracy by automatically validating patient eligibility, policy coverage, and authorization requirements in real time. Automated compliance checks ensure claims align with payer-specific regulations and documentation standards before submission, reducing avoidable denials significantly.
By combining intelligent automation, predictive analytics, and real-time validation capabilities, AI-powered billing systems help healthcare providers reduce revenue leakage, accelerate reimbursements, and create a more resilient financial infrastructure for long-term operational growth.
The Role of HIPAA-Compliant AI Agents in Healthcare Financial Operations
As hospitals continue adopting AI-powered financial technologies, maintaining regulatory compliance and protecting sensitive patient information has become a top priority for healthcare organizations. Medical billing systems process enormous volumes of confidential healthcare data every day, including patient records, insurance information, treatment histories, and payment details. Without proper security frameworks, healthcare providers risk compliance violations, financial penalties, and reputational damage.
This is why HIPAA compliant AI billing solutions are becoming essential in modern healthcare financial operations. Hospitals cannot adopt intelligent automation technologies without ensuring compliance with strict healthcare data protection standards and industry regulations. AI-driven systems handling patient and financial data must be designed with enterprise-grade security controls capable of safeguarding sensitive information throughout the revenue cycle.
Modern compliant healthcare AI systems use end-to-end encryption to secure patient data during transmission, storage, and processing. Role-based access control further strengthens security by ensuring that only authorized personnel can access specific billing information or financial records. These layered security frameworks help hospitals reduce unauthorized access risks while maintaining operational transparency across departments.
Secure cloud integrations are also playing a major role in healthcare AI adoption. Many hospitals now rely on cloud-based healthcare automation platforms that integrate with electronic health records, hospital management systems, and payer networks. To support secure healthcare automation, these platforms must follow strict compliance standards while maintaining interoperability across multiple healthcare systems.
As regulatory scrutiny around healthcare AI continues to increase, hospitals are actively investing in Compliant AI Agent in Healthcare solutions that combine intelligent automation with advanced security, privacy protection, and compliance management capabilities. Trustworthy AI infrastructure is no longer optional in healthcare finance—it has become a foundational requirement for sustainable digital transformation.

AI Agents and the Future of Intelligent Revenue Cycle Management
The future of healthcare finance is moving rapidly toward autonomous, AI-driven ecosystems capable of managing complex revenue cycle operations with minimal human intervention. As hospitals continue facing increasing reimbursement complexity, staffing shortages, and rising administrative costs, intelligent AI agents are emerging as the next evolution of healthcare financial management.
Future-ready hospitals will increasingly rely on intelligent revenue cycle management systems that can independently analyze financial workflows, optimize reimbursement strategies, and automate payer communication in real time. Unlike traditional automation platforms, modern AI agents continuously learn from historical financial data, patient billing trends, and payer behavior to improve operational decision-making dynamically.
One of the most significant advancements shaping the future of medical billing automation is the rise of conversational and voice-enabled AI systems. Voice AI technologies are expected to support billing departments by automating patient payment inquiries, insurance verification conversations, and reimbursement status updates. Conversational AI platforms may also improve patient engagement by simplifying billing communication and offering real-time payment assistance across digital channels.
Predictive reimbursement forecasting is another emerging innovation transforming AI-driven healthcare operations. Advanced AI systems can analyze historical claims performance, denial trends, seasonal healthcare demand, and payer response patterns to forecast future reimbursement outcomes with greater accuracy. These predictive insights help hospitals strengthen financial planning and reduce revenue uncertainty.
Healthcare organizations are also beginning to explore agentic AI ecosystems where multiple intelligent agents collaborate across billing, compliance, scheduling, patient communication, and operational management systems. These interconnected AI environments can streamline decision-making across departments while improving financial coordination throughout the healthcare ecosystem.
As hospitals continue modernizing their digital infrastructure, investments in scalable custom ai software development solutions and advanced agent ai development services will play a critical role in building future-proof financial automation systems capable of supporting long-term operational growth and healthcare innovation.
Why Hospitals Need Custom AI Solutions for Billing Automation
Every hospital operates with unique financial workflows, payer relationships, patient management processes, and compliance requirements. Because of this complexity, many healthcare organizations struggle to achieve optimal results using generic billing software or standardized automation tools. Modern healthcare systems require intelligent platforms capable of adapting to specialized operational needs while supporting long-term scalability and interoperability.
Custom healthcare AI solutions provide hospitals with greater flexibility to align automation systems with their existing infrastructure, billing procedures, and departmental workflows. Unlike off-the-shelf software, customized AI platforms can integrate directly with electronic health records, hospital management systems, insurance verification tools, telemedicine platforms, and patient communication applications. This seamless connectivity improves operational visibility while reducing workflow fragmentation across departments.
Scalability is another major reason hospitals are investing in customized healthcare automation platforms. Multi-specialty hospitals often manage highly complex billing structures involving different payer rules, treatment protocols, reimbursement models, and documentation standards. Generic hospital billing software may struggle to support these specialized workflows efficiently, leading to operational bottlenecks and revenue inconsistencies.
Custom AI systems also improve long-term return on investment by allowing healthcare organizations to optimize workflows based on their specific business objectives. Hospitals can automate high-volume administrative tasks, improve payer coordination, enhance claims accuracy, and streamline patient billing experiences while maintaining greater control over compliance and security frameworks.
As healthcare delivery models continue evolving, integration with mobile healthcare technologies is becoming increasingly important. Hospitals are now investing in advanced platforms that combine billing automation with telemedicine services, patient engagement tools, and digital care management systems. This growing demand is accelerating the adoption of custom healthcare mobile development and scalable custom ai software development solutions designed specifically for modern healthcare environments.
Conclusion
AI agents are rapidly transforming the way hospitals manage medical billing, insurance claims processing, and healthcare revenue cycle management. As financial operations become more complex, healthcare organizations are increasingly turning toward intelligent automation technologies to reduce administrative burdens, improve billing accuracy, and strengthen long-term financial performance.
Traditional manual billing systems often create operational inefficiencies that lead to delayed reimbursements, coding errors, claim denials, and revenue leakage. AI-powered automation is helping hospitals overcome these challenges by streamlining insurance verification, automating claims submission, optimizing coding accuracy, and improving reimbursement workflows across the healthcare ecosystem.
The impact of intelligent automation extends far beyond operational efficiency. Faster reimbursements improve hospital cash flow, while predictive analytics and AI-driven decision-making help healthcare providers reduce denial risks and maintain stronger financial stability. Advanced security frameworks and compliant healthcare AI systems are also enabling hospitals to adopt digital financial technologies while maintaining strict patient data protection and regulatory compliance standards.
As healthcare organizations continue investing in digital transformation, AI-driven revenue cycle management will become an essential component of future-ready hospital infrastructure. Hospitals that embrace intelligent financial automation today will be better positioned to improve scalability, enhance patient experiences, and maintain competitive operational performance in an increasingly data-driven healthcare industry.
The future of healthcare finance is no longer centered around reactive billing systems. It is being shaped by intelligent AI agents capable of delivering faster, smarter, and more secure financial operations across the modern healthcare ecosystem.

Leave a comment